|
canis excretory or secretory (TES) antigens, which are then confirmed via immunoblot (Ma et al. 2020).ĭiagnosis is based on clinical presentation and imaging findings as well as results from serological tests, in particular enzyme-linked immunosorbent assays (ELISA) for T. Seroprevalence in Europe spans from 2.4 to 31% (Strube et al. Generally, human toxocarosis is more prevalent in rural areas than urban ones. Worldwide, toxocarosis is one of the most commonly documented zoonotic helminth infections. and was subsequently called “common toxocarosis.” Thus, “covert” and “common” toxocarosis seem to represent the same clinical entity depending on whether a child or an adult is suffering from it (Glickman et al. A similar syndrome in adults was outlined by Glickman et al. described in children the aforementioned clinical entity as “covert toxocarosis” (Taylor et al. Based on the results of a case–control study, Taylor et al. More frequently, they develop non-specific symptoms including fever, nausea, vomiting, abdominal pain, hepatomegaly, pulmonary symptoms, lymphadenitis, limb pain, lethargy, and behavioral disorders. Generally, the majority of patients infected with Toxocara do not develop severe systemic manifestations. Neurotoxocarosis results from the migration of larvae in the central nervous system, causing meningitis and encephalitis, and commonly presents with non-specific symptoms such as fever or headache (Finsterer and Auer 2013). It is caused by larval localization in the eye and the resulting immunological response (Pivetti-Pezzi 2009). Ocular larva migrans can lead to blindness due to severe vitritis, tractional retinal detachment, or cystoid macular detachment. Additional symptoms may include lymphadenopathy, myocarditis, arthritis, and nephritis (Taylor et al. Patients often present with wheezing, coughing, pruritic urticaria-like cutaneous lesions, myalgia, and eosinophilia. Visceral larva migrans can lead to pneumonia and hepatitis as the larvae migrate through the lungs and liver, respectively. Depending on the clinical presentation, four clinical forms have been recognized: visceral larva migrans ocular larva migrans neurotoxocarosis covert, common, and cardiac toxocarosis (Auer and Walochnik 2020). Once inside the small intestine, the larvae exit the eggs, penetrate the intestinal wall, and then reach the circulation, from where they migrate to the liver, lungs, and heart, leading to an inflammatory response and clinical symptoms depending on the affected organs (Ma et al. Consumption of raw or undercooked meat from other paratenic hosts like cattle, sheep, and chickens can be a further route of transmission. Children showing symptoms of pica are therefore at high risk. Contamination of parks, playgrounds, etc., with the feces of infected animals (dogs, cats, and other carnivores) is the main source of transmission. Humans serve as paratenic hosts and acquire the infection by ingesting Toxocara eggs, which contain infective third-stage larvae (Rostami et al. 
Genetic causes have been found in 30–35% of cases of ASD and the remaining 65–70% of cases are thought to be caused by a combination of environmental factors, multiple mutations, and rare genetic variants.Īround 700,000, or one in 100, people in the UK have ASD which includes a range of conditions such as Asperger’s syndrome and autism.Toxocarosis results from human infection with larvae of the ascarid nematodes Toxocara canis and T. NHS England has released a statement on the research, which says that although the research gives an insight into whether there are detectable differences in blood and urine samples of people with and without ASD, it is far too soon to say whether such tests could ever have a role in clinical practice. However, the scientific benefits of identifying those who have autism earlier will help improve our understanding of the condition and provide greater opportunities to develop treatments and therapies.” Rapid diagnosis of autism will mean that those affected, and their loved ones, can have clarity at earliest opportunity and hopefully received the support they need. “The potential implications of this test are evident. 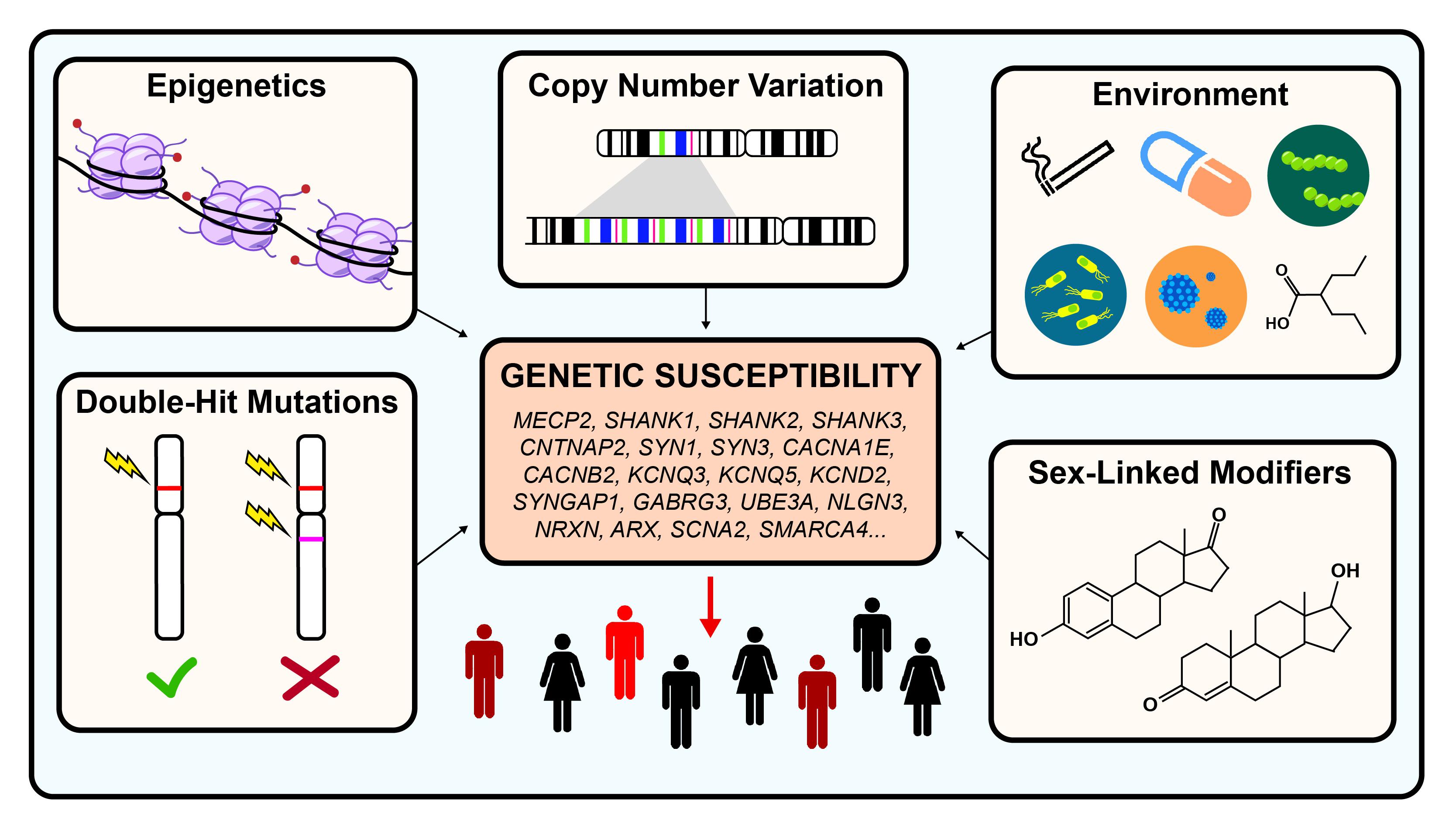
Our test has an accuracy of 88% and does not require expert behavioural observations – only a blood sample and could take weeks to diagnose. 
Current NICE guidelines use a scoring system based on test, assessing speech and cognition and observation of behaviour by a clinical experts and has accuracy of 60 – 70 and average diagnosis time in UK is 4.5 years. Lead researcher and reader of experimental systems biology at the University of Warwick Dr Naila Rabbani told Pharmaceutical Technology: “This is the first simple, blood-based test of high accuracy for diagnosis of autism.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
